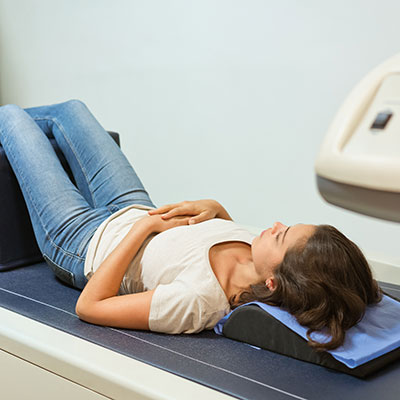
When is a Bone Density Scan Needed?
DEXA is most often used to diagnose osteoporosis, a condition that often affects women after menopause but may also be found in men and rarely in children. Osteoporosis involves a gradual loss of calcium, as well as structural changes, causing the bones to become thinner, more fragile and more likely to break.
DEXA is also effective in tracking the effects of treatment for osteoporosis and other conditions that cause bone loss.
The DEXA test can also assess an individual’s risk for developing fractures. The risk of fracture is affected by age, body weight, history of prior fracture, family history of osteoporotic fractures and lifestyle habits, such as cigarette smoking and excessive alcohol consumption. These factors are taken into consideration when deciding if a patient needs therapy.
Bone density testing is strongly recommended if you:
- Are a post-menopausal woman and not taking estrogen
- Have a personal or maternal history of hip fracture or smoking
- Are a post-menopausal woman who is tall (over 5 feet 7 inches) or thin (less than 125 pounds)
- Are a man with clinical conditions associated with bone loss
- Use medications that are known to cause bone loss, including corticosteroids such as Prednisone, various anti-seizure medications such as Dilantin and certain barbiturates, or high-dose thyroid replacement drugs
- Have type 1 (formerly called juvenile or insulin-dependent) diabetes, liver disease, kidney disease or a family history of osteoporosis
- Have high bone turnover, which shows up in the form of excessive collagen in urine samples
- Have a thyroid condition, such as hyperthyroidism
- Have a parathyroid condition, such as hyperparathyroidism
- Have experienced a fracture after a mild trauma
- Have had x-ray evidence of vertebral fracture or other signs of osteoporosis